The role of the international community in current crises in the Central African Republic and northern Nigeria may be mired in confusion, but it can do something about the Ebola epidemic in west Africa.
The outbreak of the virus, which started in Guinea and has spread to Liberia and Sierra Leone, is the deadliest in recorded history, with Médecins sans Frontières (MSF) and the World Health Organisation (WHO) declaring the situation out of control.
There are more than 759 cases across 60 sites since the first ones were confirmed in March – that's almost 50 known cases per week and a 20% increase in cases since 23 June. Almost 500 people have died from the disease, which has spread across international borders.
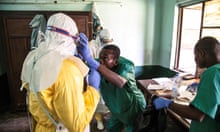
Ebola has a fatality rate of up to 90% – once you have it, your chances of survival may be just one in 10. There is no vaccine and no cure; the only way to stop the virus is to prevent it or treat the symptoms if diagnosed early enough. It is primarily spread by contact with the blood or body fluids of an infected person and in some cases by contact with dead animals (primarily monkeys and bats) which are infected.
But here is where the international community can help. The health systems in west African countries are weak: three countries ranked 174 (Liberia), 177 (Sierra Leone) and 178 (Guinea) out of 186 countries for human development, according to the UN development programme. So, one of the world's most deadly viruses is plaguing three of the countries least equipped to cope with it.
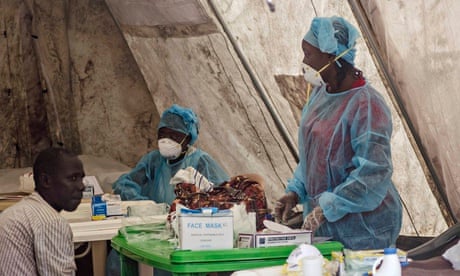
In Sierra Leone, I have been involved in a two-year research programme to prevent malnutrition. This has involved spending time at some of the government-run peripheral health units (PHUs) in northern Sierra Leone, on the border with Guinea. The PHUs are the frontline of healthcare – assuming, of course, you can reach one of the 1,228 clinics across the country (one community we visited is a 6km walk from the nearest PHU). When access to state health services is limited; locals often turn to traditional healers, who sometimes misdiagnose Ebola and treat it as a curse.
The PHUs are critical in providing immunisations, malaria treatment, delivering babies, providing free medical care to pregnant and lactating mothers and children under five – but they are not without serious problems. Staff often lack good-quality training, partly because they tend to learn through cascade models, where one person might train 10 others, who in turn train 10 more, and so on – operating like a system of Chinese whispers with all the potential miscommunication this can involve.
There is a high turnover of PHU staff owing to poor working conditions: for example, nurses earn just $55 (£32) per month – roughly $1.80 per day – meaning that new, untrained staff are commonly found at the frontline of Sierra Leone's healthcare system. A lack of quality training means staff are not always equipped to deliver appropriate healthcare messages or treatment. In fact, such professionals make up a large number of those who have died in the Ebola outbreak, having failed to take precautions in dealing with infected patients. The PHUs often face shortages of equipment and medicine.
To bring the virus under control, countries need more help from external partners. In the immediate term, emergency humanitarian support is needed to treat those infected and prevent further cases; MSF says it has reached its limit and that a massive deployment of resources is required. If donors and individuals want to support aid that shows tangible results in relatively short timeframes, supporting the response to the Ebola virus seems a good option that could save potentially thousands of lives.
In the longer term, support must focus on building the capacities of national health and sanitation systems to respond to emergencies and prevent such unnecessary loss of life. Ebola is not the first disease to wreak havoc in this region. Less than two years ago, Guinea and Sierra Leone faced a cholera outbreak that killed 392 people.
Prevention might be better than cure, but it is also much harder to build capacity to do this. This is because preventative capacity is not only about technical knowledge, but about how well the different parts of health and sanitation systems work together and interact with local dynamics, such as preference for tradition healers or stigma, for example.
Building this capacity to prevent future health emergencies is a long-term endeavour that becomes more critical with each epidemic in the region.
Lisa Denney is a research fellow in the politics and governance programme at the Overseas Development Institute. She leads the Secure Livelihoods Research Consortium's country programme in Sierra Leone








Comments (…)
Sign in or create your Guardian account to join the discussion